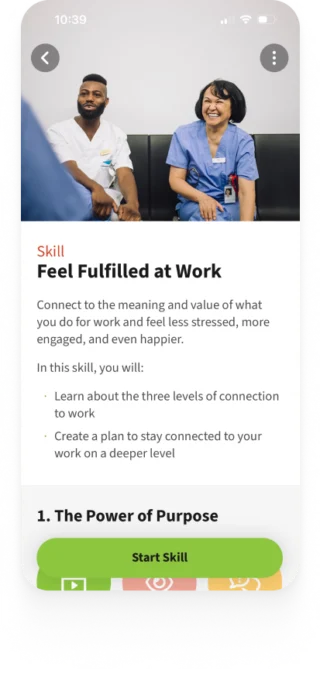
meQ detects compassion fatigue and attrition risk in advance, helping prevent unplanned turnover and protecting the patient safety that depends on a stable health systems workforce.
meQ is built for the full spectrum of your workforce: from bedside nurses and OR teams navigating acute trauma and shift fatigue, to physicians managing cognitive overload, to administrative staff facing their own distinct pressures.
Nurses face some of the most acute workforce pressures in healthcare today, eroding specific resilience factors — Empathy, Emotion Control, Energy, and Sleep. meQ targets those factors directly, rather than delivering the generic stress-management content most platforms treat clinical workers with.
Leading a high-performing clinical team takes more than expertise; it demands emotional intelligence, the ability to coach under pressure, and the agility to keep teams connected and productive through constant change. meQ gives charge nurses and unit managers the upskilling tools to build exactly those skills, delivering science-backed micro-learning in the flow of work rather than through time-consuming training programs.
Long surgical blocks, unpredictable emergency volumes, and sustained cognitive demand create a distinct stress profile. meQ helps these teams maintain decisiveness, focus, and physical recovery across shifts that don't fit into a standard schedule.
meQ gives operations leaders the visibility to understand where resilience is eroding across their organization — and the data to make smarter, faster decisions about where to intervene.
At the same time, meQ supports administrators' own resilience, delivering targeted skill-building around decision fatigue, cognitive load, and leadership under uncertainty, so the people responsible for holding the system together have the tools to sustain themselves while they do it.
Nurse turnover is the most expensive workforce problem in healthcare, and clinician burnout doesn't just drive attrition, it impacts patient safety.
meQ integrates with nurse scheduling, leave management, and workforce planning systems — so resilience data informs staffing decisions, not just wellness reports. Your planning team sees which units are trending toward turnover before the schedule gaps become patient safety risks.
Reduction in
depression risk
Lower
turnover
Decrease in workforce
burnout risk
meQ helps health systems detect early signs of burnout, support the teams that carry patient outcomes, and protect the retention and safety metrics your healthcare CFO actually tracks.
Healthcare professionals face distinct cognitive pressures, from moral injury to compassion fatigue to split-second decision-making under resource constraints. meQ addresses this by prescribing skills based on each individual's specific stress profile, so a bedside nurse receives different support than a department director.
Many health systems position meQ's self-service, actionable content as a practical performance tool, not a mental health initiative. Focusing on a small group of highly engaged "power users," such as charge nurses or unit managers, can create organic adoption that spreads across the organization.
Unlike traditional wellness apps, meQ translates "soft" metrics into hard business outcomes, connecting clinical burnout data to turnover costs, vacancy rates, agency spend, and patient satisfaction scores. It makes the case that supporting individual resilience is a direct investment in workforce stability and care quality.
meQ complements your existing EAP by acting as an intelligent "front door" that makes your current investments work harder. When meQ's predictive assessments detect that an employee is showing high-acuity risk, such as severe anxiety, compassion fatigue, or crisis indicators, the platform routes them directly to your existing EAP or relevant point solutions, ensuring no one falls through the cracks.
If you need a comprehensive solution, meQ offers a fully integrated EAP that covers the entire acuity continuum within a single platform. This prevention-first approach starts with everyday digital resilience training and manager enablement for low-to-moderate stress, but seamlessly scales to high-acuity clinical care when employees need it.
Our integrated EAP provides access to master's-level counselors, direct connections to clinical therapists, and critical incident support — so if a mass layoff, workplace trauma, or patient crisis occurs, meQ can deploy experts for on-site support and leadership coaching within 24 hours.
Compassion fatigue is an occupational hazard with a specific clinical signature — chronic exposure to suffering, death, and moral injury erodes four named resilience factors: Empathy, Emotion Control, Energy, and Sleep. meQ's 18-factor clinical model measures these directly and delivers targeted interventions for each, rather than the generic stress-management content most wellness platforms deliver to clinical populations.
Yes. An ICU nurse's burnout pattern (Empathy collapse, moral injury) looks different from an OR nurse's (physical depletion, sleep disruption) or a billing department's (Purpose erosion). meQ recognizes these distinct patterns across clinical and support populations, and delivers interventions matched to each role's actual stress profile rather than treating every healthcare employee the same.
meQ delivers 5-to-10-minute micro-learning moments through mobile channels, timed to each clinician's individual schedule. Sleep interventions arrive when they're biologically relevant, recovery content lands after the shift actually ends, and engagement fits into the five-minute gap between patient rounds — not a 30-minute module that assumes a desktop and a lunch break.
Healthcare has one of the clearest retention ROI cases in any industry. A departing nurse costs $56K–$89K to replace; a physician costs $500K–$1M. meQ maps resilience decline directly to attrition probability, flags retention risk before it becomes a resignation, and translates outcomes into the metrics a self-insured health system CFO actually tracks — retention cost avoidance, medical cost reduction (typically 10–15%), and absenteeism reduction. Utilization reports like "300 people used the EAP" don't answer the CFO's question. Dollar-denominated retention data does.
meQ embeds into nurse scheduling, leave management, and workforce planning infrastructure — so resilience data feeds directly into the staffing decisions your team is already making. Workforce planning sees not just who's out today, but which units are likely to be short next month and where retention risk is concentrating.
Yes, and meQ makes your existing benefits work harder for you. EAPs and peer support are reactive; they activate after someone raises their hand. By the time a nurse running on depleted sleep and eroded stress management calls the EAP, they're usually past the point of retention. meQ surfaces the resilience signal 60 to 90 days earlier and routes high-acuity risk into your existing EAP and clinical partners, extending the reach of programs you've already invested in.
Connect with our team see how meQ can support your organization.